How to successfully perform spirometry

Spirometry is a basic method of assessing lung function. Are you a medical professional looking to refresh your knowledge? This guide offers a comprehensive overview of topics – from basic concepts in spirometry to the most commonly diagnosed conditions and advancements in its technology. We are also welcome to download a free e-book!
In this blog you will learn:
1. How spirometry works
What is spirometry?
When to perform spirometry?
What kind of conditions can it detect?
What does spirometry measure?
2. How to conduct a spirometry measurement
3. Frequently diagnosed conditions in spirometry
4. Automatic tools in spirometry
5. A comparison of different spirometry devices
How spirometry works
What is spirometry?
Spirometry is the basic method of assessing how well your lungs work. It is a simple non-invasive diagnostic test that measures:
how much air the patient can breathe in and then breathe out with maximum effort.
how easily and how fast the patient can breathe the air out with maximum effort.
When to perform spirometry?
Spirometry is performed at different levels of healthcare. We use it to:
Detect, follow and manage lung disorders [3]
When a lung disease is discovered or suspected, spirometry helps diagnose it, measure its effects on lung function, assess airway responsiveness, monitor the effect of prescribed therapy, analyse pre-operative risks, and make a prognosis.
Assess risk exposures
Spirometry is used for monitoring adverse effects of medications known for pulmonary toxicity or the impact of exposures to injurious substances.
Check the general lung status
Spirometry helps assess an individual’s pulmonary health, e.g. before employment (especially at-risk occupations) or before activities with physical risk.
What kind of conditions can it detect?
Among others, spirometry is used in the detection of the following conditions: [4]
Obstructive lung disorders
They cause airflow blockages and breathing problems (e.g. asthma, COPD).
Restrictive lung disorders
They limit the expansion of the chest wall or lung elasticity; this decreases the air volume that the patient can breathe in (e.g. sarcoidosis, pulmonary fibrosis).
Cardiovascular risk
This risk can arise due to lung complications, and includes coronary artery disease (CAD) and heart attack. [5]
What does spirometry measure?
The mechanics of breathing
The lung is an elastic organ. When we breathe in, the diaphragm and other muscles involved in respiration contract, making the chest cavity expand. This expansion causes a negative pressure within the lungs, which draws air in. [6] [7] [68]
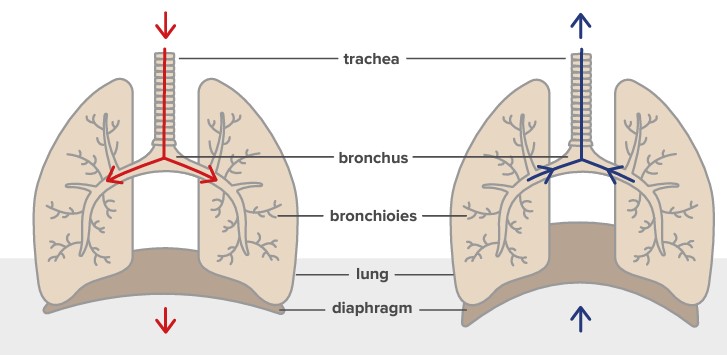
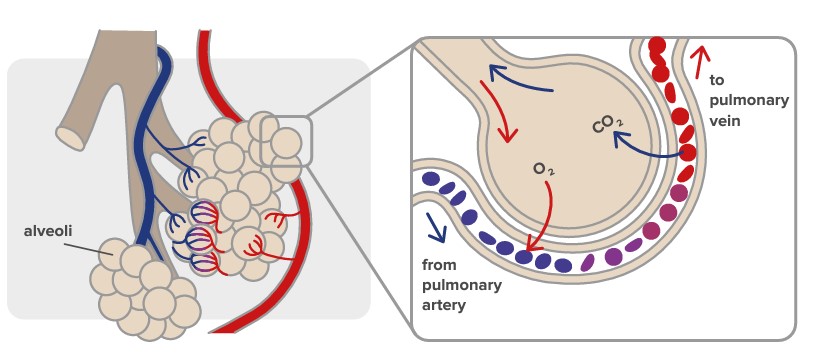
As we INHALE, air goes down the trachea and enters the lungs via two large tubes called bronchi. In the lungs, bronchi divide into many small tubes known as bronchioles, resembling the branches of a tree. The bronchioles terminate in clusters of tiny air sacs called alveoli. These have delicate walls containing a network of tiny blood vessels. When we breathe in, oxygen from the inhaled air diffuses into these vessels and enters the bloodstream.
During EXPIRATION, the muscles relax, and carbon dioxide, a waste product of metabolism, is expelled. For this, the elasticity of the alveoli and the bronchial tubes is essential.
How to conduct a spirometry measurement
Spirometry involves a series of steps and considerations for accurate respiratory measurements. Here is a short outline, but click here for a comprehensive article:
The process begins with device preparation and calibration to guarantee precise readings, followed by selecting appropriate prediction models for reference values. Patient preparation is also crucial to ensure reliable results. During measurement execution, either open-loop or closed-loop spirometry can be utilised. In interpreting the result, the Z-score can be used – a mathematical combination of the percent predicted value and the variability observed between individuals.
Acceptability criteria dictate that at least three acceptable maneuvers are required, with reproducibility criteria ensuring the best two maneuvers are consistent. In this, repeatability and acceptability criteria, along with a maximum of eight maneuvers, should be used as prescribed by the local and international guidelines.
Time, volume and flow
These are the three basic measurements in spirometry. In order to test them, the patient performs a series of breathing techniques or actions called maneuvers.

TIME
In spirometry, the most important aspect of time is usually the length of the expiration. Depending on what we are investigating, the patient should either expire as forcefully and completely (FVC maneuver) or as slowly and steadily as possible (SVC maneuver). In either case, the patient should expire for as long as they can.
For reliable results, a maximum effort and a steady airflow without interruptions are needed. During the maneuver, we usually encourage the patient to go on, with words like “more, more, more”.
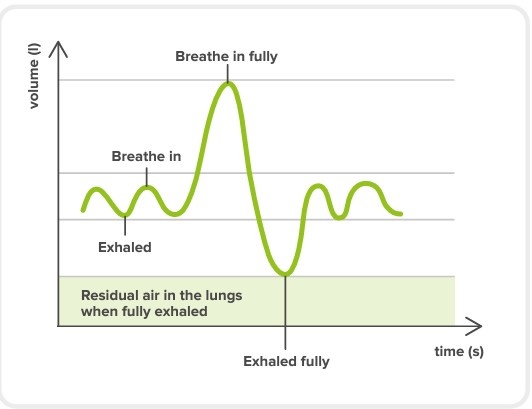
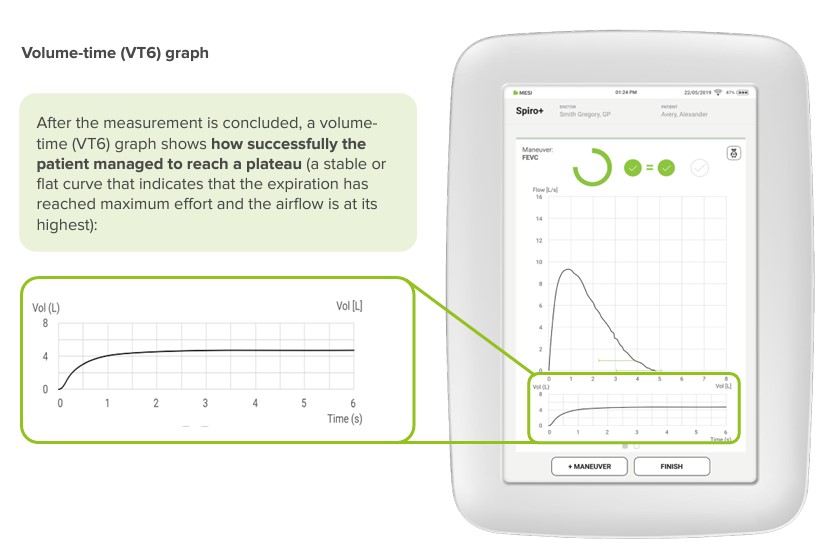
The graph shows the time on the x axis and the air volume (inspired/expired) on the y axis. [7]
VOLUME
Volume refers to the measurement of the amount of air the patient inspires or expires during various maneuvers.
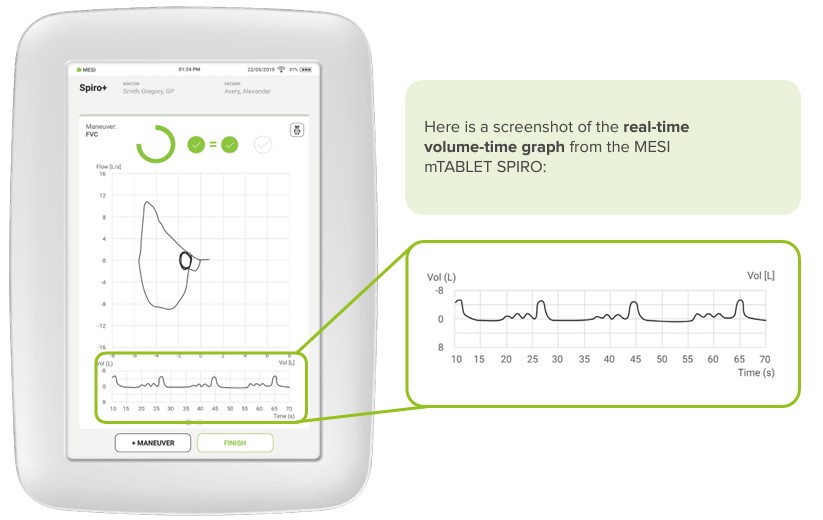
Real-time volume-time graph
The real-time volume-time graph is used to observe live breathing patterns during the procedure, showing the following measurements:
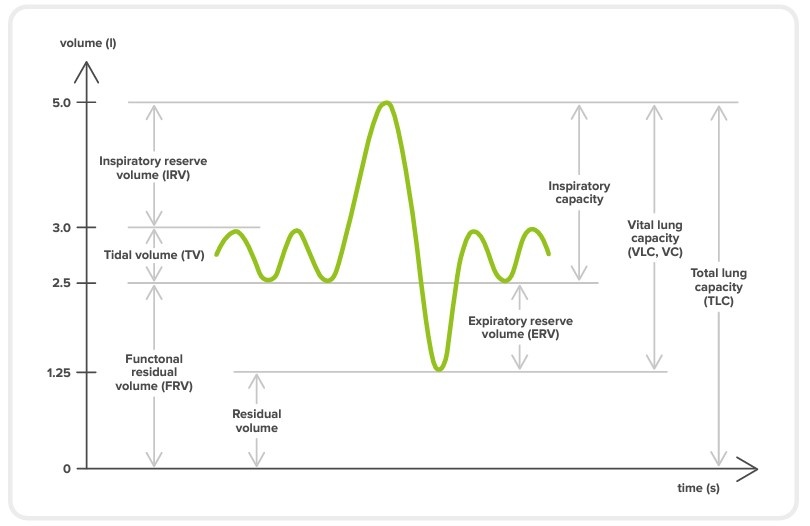
Inspiratory reserve volume (IRV): The amount of air that can be inspired with maximum effort after a normal (passive) inspiration.
Tidal volume (TV): The amount of air moved into or out of the lungs during inspiration or expiration while the patient rests (and breathes normally/passively).
Functional residual volume (FRV): The amount of air that remains in the lungs at the end of a normal (passive) expiration.
Expiratory reserve volume (ERV): The amount of air that that can be expired with maximum effort after a normal (passive) expiration.
Residual volume (RV): The amount of air that remains in the lungs after a maximum expiration.
Vital lung capacity (VLC, VC): The maximum amount of air slowly expired from a fully inflated lung (after the deepest inspiration).
Total lung capacity (TLC): The maximum volume of air in the lungs after a maximum inspiration.
For a full list of definitions of spirometry measurements, click here.
FLOW
Flow refers to the rate (speed) at which air moves in or out of the lungs in breathing maneuvers.
The flow-volume graph or loop displays flow (in L/s) and how it relates to lung volume (in L) during:
maximal inspiration from complete expiration and
maximum expiration from complete inspiration.
Here are some things that we can measure with it: [8]
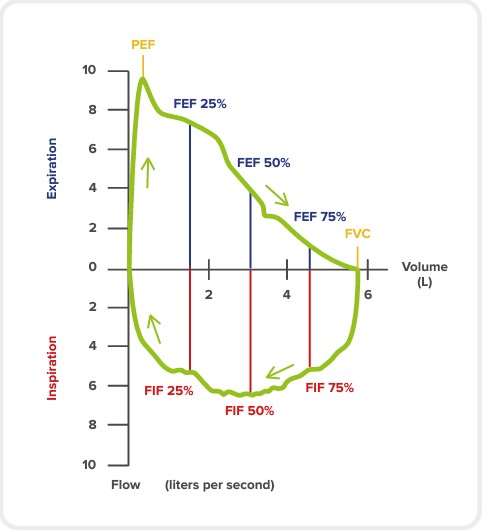
For a full list of definitions of spirometry measurements, click here.
Is the spirometry result always accurate?
The spirometry procedure should ensure that the measurement is:
objective,
non-invasive,
sensitive to fast change and
reproducible.
Technology advancements, especially digital spirometers, have made spirometry simpler and much more reliable than in the past. However, there are always a few factors to consider. [2] [3] [11]
Firstly, the test itself largely depends on patient cooperation and effort. Secondly, the diagnosis of pulmonary conditions may be a long and complex process; their symptoms often overlap, also with non-pulmonary illnesses. [9]
For these reasons, spirometry is always used together with other physical findings, symptoms, and the patient’s history.
What are the contraindications for spirometry?
DISCLAIMER: The list of the contraindications below may change over time and is not exhaustive. Before performing spirometry, please consult the latest guidelines.
Absolute contraindications
Recent myocardial infarction or acute coronary syndrome
Respiratory infection, a recent pneumothorax or a pulmonary embolism
Hemodynamic instability (abnormal or disrupted cardiovascular function resulting in inadequate blood flow)
A growing or large (> 6 cm) aneurysm of the thoracic or abdominal aorta
Acute hemoptysis (coughing up blood)
Retinal detachment
Intracranial hypertension
Relative contraindications
Conditions that make it difficult to hold the mouthpiece (e.g. pain in the facial area)
Patients who can not be instructed to use the device properly (patients with dementia, small children)
Hypertensive crisis (sudden, severe blood pressure increase)
Recent thoracic, abdominal, eye, ear, throat, nose or brain surgeries
Frequently diagnosed conditions with spirometry
The most common conditions diagnosed by means of spirometry fall into two categories. For a detailed description of their symptoms, treatment, detection and how they differ from normal lung function, click here:
Obstructive conditions:
Asthma
Chronic obstructive pulmonary disorder (COPD)
Bronchitis
Emphysema
Cystic fibrosis
Bronchiectasis
Restrictive conditions:
Pneumonitis
Pulmonary fibrosis
Sarcoidosis
Automatic tools in spirometry
The success of spirometry measurements very much depends on the patient's effort. However, digital technology can help both the patient and the clinician in the examination. The MESI mTABLET SPIRO offers a great number of digital features to make your work easier and faster. Click here to find out more about the following:
a real-time display of the flow-volume curve, ensuring you can monitor and guide the patient effectively,
maneuver quality warnings alert you to any issues,
BestBreath™ technology for automatic selection of the best results (but you can also choose them manually if you wish), and
animated incentive mode for paediatric use.
A comparison of different spirometry devices
There are different types of spirometry devices on the market. The most common ones are desktop spirometers and PC-based spirometers.However, new-generation digital spirometers are among the most effective. The MESI mTABLET SPIRO is the most versatile digital spirometer – with many systemic advantages and extra highlights for different levels of healthcare. For a detailed comparison of different types of spirometers in terms of their use, software, mode of operation, extension possibilities and calibration, click here.
Here is a user-friendly SPIROMETRY e-book full of illustrations!
 Get your free copy here
Get your free copy here