- DE
- EN
- ES
- FR
- IT
- SL
Incidence of diabetes is on the rise and it is projected that this trend will likely continue in the future. The socioeconomic burden grows concurrently and many healthcare organisations and practitioners are having great difficulties providing treatment for a broad spectrum of symptoms and conditions associated with this chronic metabolic disorder.
It is estimated that there are about 425 million people with diabetes worldwide and if the prevalence rate remains unchanged for the foreseeable future, their number will increase to at least 629 million by the year 2045 [1]. That’s assuming that existing and potential new preventive measures don’t bear fruit and lower the incidence rates, together with disability and mortality rates. And the current picture for the latter is far from rosy: in 2016 there were at least 1.6 million deaths directly associated with diabetes [2]. Mortality aside, diagnosis of diabetes (both type 1 and type 2) is associated with a significant impact on the patient’s quality of life (dependent on the severity of the disease). Possible complications range from erectile dysfunction and (diabetic) neuropathy to diabetic retinopathy and diabetic foot, which is the topic of this blog post.
Diabetes foot care
Diabetic foot is a complex lower extremity condition caused by long-term hyperglycaemia and varies in its severity in accordance with management of diabetes itself and presence of other medical conditions, particularly of a cardiovascular nature such as PAD. Naturally, these additional factors further aggravate damage done by other complications of diabetes such as neuropathy, which leaves the patient with diminished sense of pain, opening the door for sores and blisters and subsequent infections – diabetic foot ulcers. Those are usually difficult to treat as the normal healing process is disrupted by changes in metabolism brought on by diabetes and diminished vascular flow of nutrients and oxygen (due to hyperglycaemia-accelerated atherosclerosis).
Before we delve into a list of recommendations general practitioners (and diabetologists) should convey to their diabetic patients to mitigate the risk of such complications, we had better dedicate a word or two to statistics surrounding epidemiology and symptomatology of diabetic foot, including the most significant comorbid conditions.
The most common pathology of diabetic foot are diabetic foot ulcers, which affect between 15 to 25% of diabetics during their lifetime [3].
Their manifestation is clinically significant not only from the difficulties connected with their treatment and fighting infections, but also the simple fact that they very often precede lower-leg amputations. Estimates go as high as 84% – it also has to be noted that the diagnosis of diabetes itself holds 15 to 20 times greater risk of amputation (in comparison to risk in healthy, non-diabetic individuals) [4]. Amputation as such carries significant mortality, ranging from 39 to 80% in a 5-year period after diagnosis [5]. However, patients with comorbidities such as PAD fare considerably worse in that regard [5]. At least 20% of diabetics have (symptomatic) PAD, but this number is generally recognised as being an underestimate since PAD is often entirely asymptomatic, hindering timely diagnosis (in the absence of modern diagnostic tools) [6].
Regarding other comorbid medical conditions: there are quite a few of them, most of them affecting the cardiovascular system, like the aforementioned PAD, but few as dangerous as coronary artery disease (CAD), the biggest killer amongst cardiovascular diseases (CVDs) and by itself [7] Rates of morbidity and mortality related to CVDs as such are 2 to 4 times higher in diabetics (type 2) than in non-diabetics [8]. Besides that, there are considerably higher rates of disability and degraded quality of life amongst diabetics than non-diabetics. Still, there is much that can be done to alleviate or even (to some extent) prevent the detrimental effects of various symptoms and complications, such as diabetic foot, on the patient’s health.
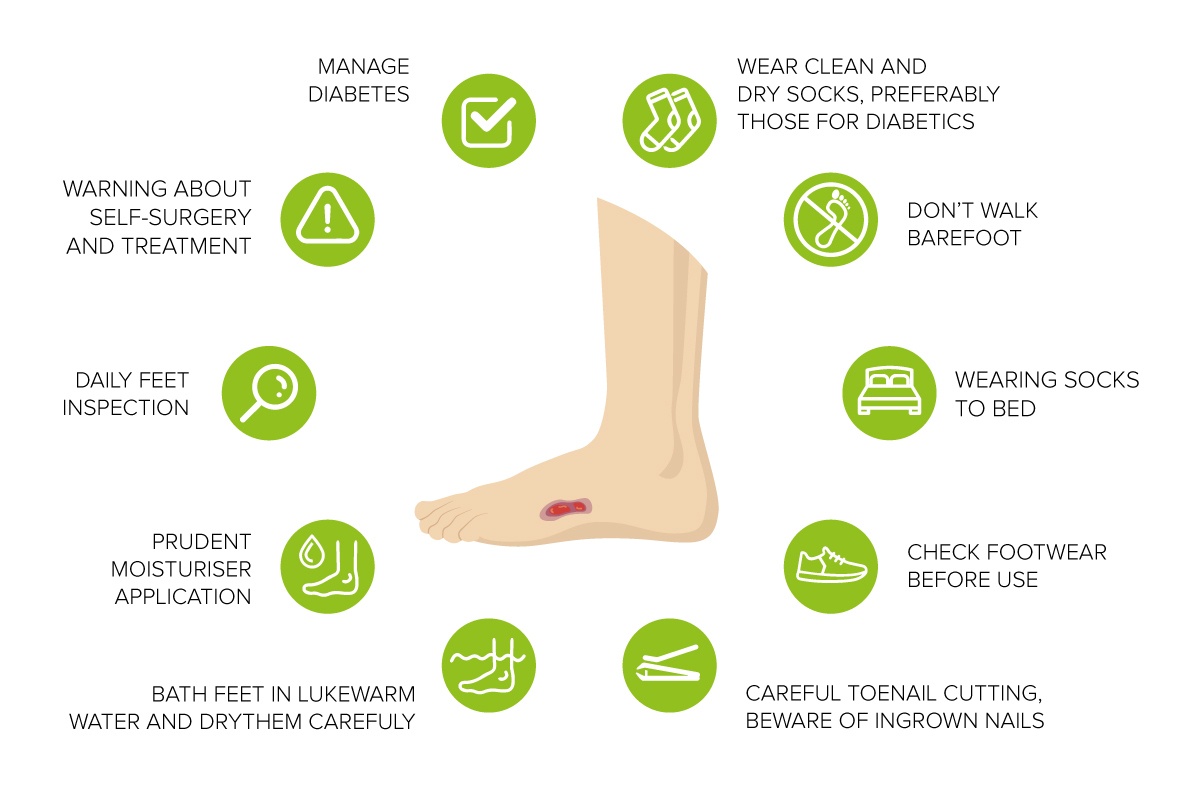
List of common recommendations to convey to diabetic patients (with diabetic foot):
- Manage diabetes. Presenting diabetic patients with a list of complications associated with diabetic foot might reinforce good practices for managing blood sugar levels.
- Daily feet inspection. Even minor foreign objects in shoes or socks can cause sores and blisters, which can quickly progress to open wounds. Patients or their carers should look for blisters, cuts, redness, swelling or issues with nails (infections) and immediately notify their personal physician or diabetologist if they notice anything.
- Bathe feet in lukewarm water and dry them carefully. Patients should avoid hot water and vigorous scrubbing with a towel.
- Prudent moisturiser application. Patients are recommended to moisturise skin on feet (to prevent cracking), with the exception of space between the toes as this could encourage fungal infections.
- Careful toenail cutting. Beware of ingrown nails.
- Wear clean and dry socks, preferably those for diabetics. Wet socks and other footwear promote chafing. It is also worth investing in socks designed especially for diabetics: they have extra cushioning and usually don’t have elastic tops.
- Wearing socks to bed. Patients who get cold feet at night should wear socks and abstain from using hot water bottles or other heating devices, which might do more harm than good.
- Check footwear before use. Patients should be reminded not to just check their feet, but likewise their footwear for any signs of wear and tear or the presence of foreign object that might cause issues.
- Warning about self-surgery/treatment. Patients have to be discouraged from treating their own blisters or any other types of wounds.
- Don’t walk barefoot. This goes without saying, particularly if the patients have inclinations to not wearing footwear in hot weather – remind them about the possibility of cuts and other types of damage.
General physicians should also inspect the feet of their diabetic patients at every general examination, even if the patients themselves have not reported any issues, and at the same time be cognisant of symptoms of possible comorbid conditions that might yet be undiagnosed, but could cause serious issues, either by further aggrandising existing complications of diabetes or on their own.
What to advise a patient with diabetic foot?


