Hypertension and Peripheral Artery Disease (PAD)
Peripheral Artery Disease (PAD) has many risk factors, but some of them are more prominent than others, such as smoking, which is the single greatest modifiable risk factor for PAD and many other Cardio-vascular Diseases (CVDs). Another risk factor, which is frequently mentioned in the same breath as smoking, for PAD and CVDs in general, is hypertension.
Hypertension is a very common medical condition and it was estimated that in 2010 about 1.39 billion individuals had elevated blood pressure (defined as average systolic blood pressure above 140 mm Hg and average diastolic blood pressure above 90 mm Hg) [1]. At the same time it is also the leading risk factor for morbidity and mortality (not a cause by itself) accounting for 9.4 million deaths in 2010 alone due to its association with virtually all CVDs which are the leading cause of mortality worldwide [2,3]. More specifically Coronary Artery Disease (CAD) – is culpable for 8.92 million deaths in 2015 [4].
Why is Coronary artery disease (CAD) even mentioned in an article about the link between hypertension and Peripheral Arterial Disease (PAD)?
Well, there is a significant comorbidity between PAD and CAD, as many patients (prevalence from 22 % to 42 %) with CAD also have PAD and they fare worse, health and mortality-wise, than those with only CAD [5,6,7,8]. PAD itself has been recognised as a clinically significant predictor of overall cardiovascular health (presence of atherosclerosis in arteries of lower extremities can be indicative of its presence in other arterial beds). Furthermore, individuals with PAD are at a significantly higher risk of mortality in general, with estimates of 5-year mortality in the region of 30 % (versus 10 % for control group without PAD) – approximately 75 % of deaths are of cardiovascular nature [9].
The answer is of course atherosclerosis – the underlying mechanism of both CAD and PAD and the effect of hypertension on atherosclerosis. The exact mechanism behind the contribution of hypertension to atherogenesis has yet to be fully elucidated, but it is suspected that it involves abnormalities in platelet activation and fibrinolysis, endothelial cell dysfunction and abnormal levels of haemostatic factors [10,11].
Given its association with atherosclerosis it is therefore not surprising that hypertension is fairly prevalent in PAD patients (35 % to 55 % of diagnosed individuals) [11]. Clinicians should be cognisant of this fact when they are examining a patient who is hypertensive or is in any other risk group for PAD.
The Effects of Hypertension on Peripheral Arterial Disease (PAD)
Despite strong association between hypertension and PAD, most clinicians fail to detect the latter in hypertensive patients unless they exhibit symptoms that are typical for the disease. Namely, only 2 % to 5 % of them have intermittent claudication (a prevalence that increases with age)[11].
But there’s more; studies have shown that subclinical PAD is common in hypertensives even in the absence of other comorbidities [12]. It has therefore been recommended that hypertensive patients are screened for PAD to identify those at an increased cardiovascular risk (especially those with a pulse pressure above 65 mm Hg) [12].
A Comprehensive Diagnostic Solution
The quickest and most cost-effective way of diagnosing PAD is on the basis of an ABI measurement which, up until recently, required skilled examiners, lest there was a likelihood of misdiagnosis, and took a considerable amount of time, which limited its potential for large scale preventive screening [13]. There are now far better tools, not only for ABI measuring, but also for assessing cardiovascular health in general. The MESI mTABLET, in combination with appropriate modules, offers a comprehensive diagnostic solution for PAD and other indicators of cardiovascular health.
The modular design of MESI mTABLET enables the clinicians to easily perform a number of diagnostic tests in a successive manner, if the previous test or initial physical examination have indicated possible cardiovascular issues (this is quite common when it comes to cardiovascular health due to the interlacing nature of indicators). For example, a clinician can measure a patient’s blood pressure (using the MESI mTABLET BP module) and determine that his/her blood pressure is elevated in comparison with the value (saved in mRECORDS) from the previous visit or has been hypertensive from the start.
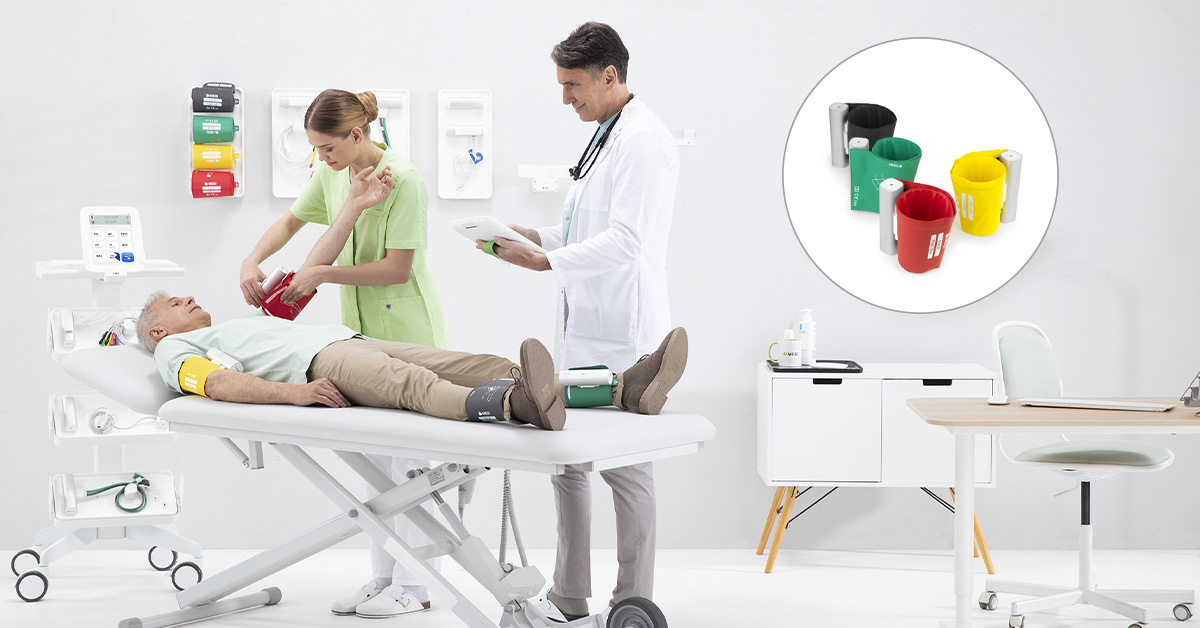
If he suspects possible PAD, either on the basis of hypertension diagnosis or patient’s inclusion in risk group(s) for PAD, he can instruct the patient to assume a supine position on the examining table before performing an ABI measurement using the pressure cuffs in the MESI mTABLET ABI module package. Results of assessment are then saved in the patient’s electronic record (mRECORDS) and can be shared with other healthcare professionals for either second opinion or as part of assessment for additional testing or treatment, if the patient has been sent to a specialist (e.g. vascular surgeon). Diagnosis of both hypertension and PAD should not be taken lightly as it can have serious short and long term complications for the affected individual.
Importance of Peripheral Arterial Disease (PAD) Measurement in Hypertensive Individuals
Screening for PAD in hypertensive patients is not only paramount from the perspective of PAD itself, but also from that of overall cardiovascular health, since those with both diseases suffer worse outcomes than those with only one. Patients with hypertension and PAD are at a greatly increased risk of myocardial infarction and stroke[11]. The comorbidity of hypertension and PAD with other medical conditions also has detrimental effects beyond those directly connected with cardiovascular health.
Studies have shown an association between hypertension and a low ABI score (diagnosis of PAD), with a decline in cognitive functions in overweigh and obese individuals with type 2 diabetes[14]. The effect on overall mortality is also distinctly negative. The cumulative death ratio (over a 5-year period) for hypertensive patients with PAD was twice as high (regardless of gender) in comparison with those without PAD[15]. Additionally, while hypertension can be managed with antihypertensive drugs (in addition to other treatments such as lifestyle modification) there is no concrete evidence that antihypertensive therapy leads to a reduction of PAD incidence [11].
Healthcare professionals are recommended to screen hypertensive patients for PAD on the basis of Ankle-Brachial Index (ABI) measurement as the health and mortality outcomes are worse for those with both diseases than for those with either.
Send inquiry