Peripheral Arterial Disease (PAD) and Diabetes
Peripheral Arterial Disease (PAD) has significant comorbidity with specific medical conditions, particularly those of cardiovascular nature like coronary artery disease (CAD), but there is another, equally serious disease that even increases the incidence of PAD and aggravates the existing one. We are talking about diabetes, which is a detrimental and complex disease on its own.
There are no exact statistics about the global prevalence of PAD due to the often asymptomatic nature of the disease (40% of patients having no symptoms, about 50% having symptoms that could be attributed to other medical conditions and only 10% having classic symptoms), but it is estimated that there were more than 202 million individuals with PAD in 2010 [1, 2, 3].
Today that number is likely far higher, whether due to the greater awareness about the disease and proliferation of modern diagnostic tools, or the fact that the world population, particularly in developed countries, is rapidly ageing (advanced age is a risk factor for PAD).
Another and very important risk factor for PAD is diabetes.
Namely, at least 20% of diabetics have (symptomatic) PAD, but this number is generally recognised as being an underestimate since PAD is often entirely asymptomatic (can only be accurately diagnosed using modern diagnostic tools) [4] .
The most typical symptom of PAD (if the disease is symptomatic), intermittent claudication, is 3.5 times more prevalent in male and 8.6 more prevalent in female diabetics than in non-diabetics (of respective genders) [5].
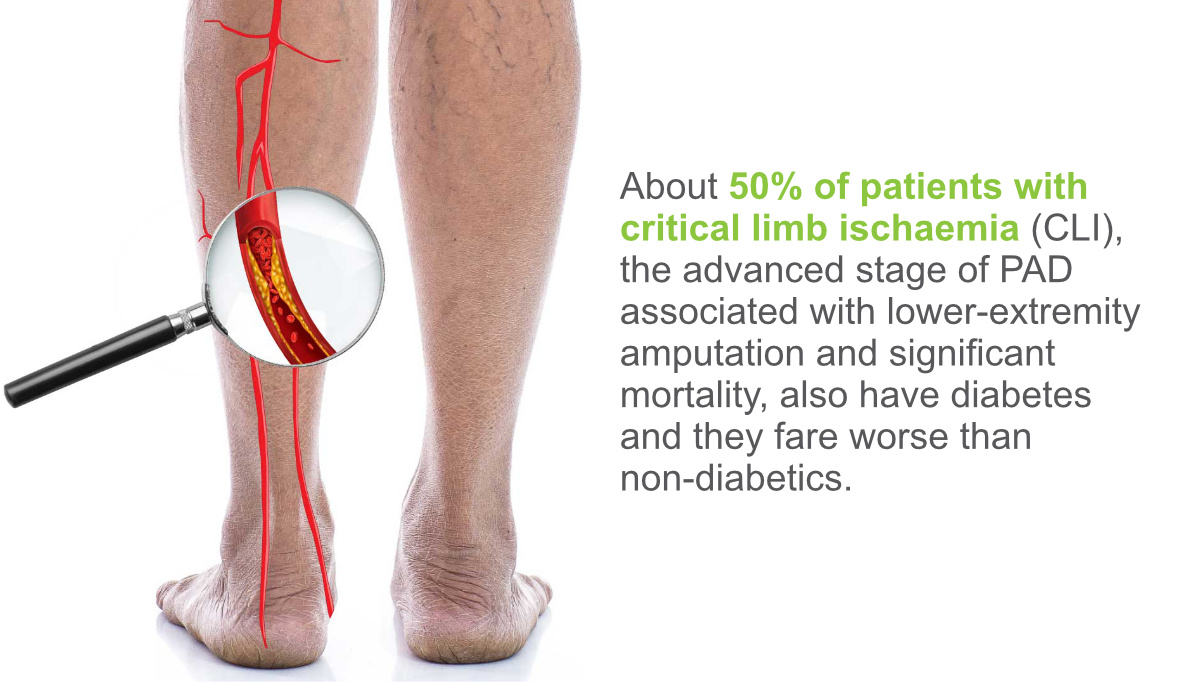
Even more, about 50% (some studies suggest an even higher number of 76%) of patients with critical limb ischaemia (CLI), the advanced stage of PAD associated with lower-extremity amputation and significant mortality, also have diabetes and they fare worse (more severe CLI) than non-diabetics [6, 7, 8].
How does diabetes increase the chance of development of Peripheral Arterial Disease (PAD)?
Why exactly is diabetes a risk factor for PAD and how does it contribute to the development and worsening of symptoms and complications of PAD?
The underlying mechanism of PAD is, of course, atherosclerosis, which can be induced by diabetes through complex, multifactorial mechanisms, which will be presented in the next few paragraphs. It should also be noted that the severity of these abnormalities increases with worsening blood glucose control and the overall duration of diabetes.
Diabetic patients have elevated serum C-reactive protein (CRP) levels, which is an important biomarker for inflammation and a cardiovascular risk factor [9, 10]. It is hypothesised that CRP may have a direct pathophysiologic role by promoting production of procoagulant tissue factor, leukocyte adhesion molecules, and chemotactic substances.
Additionally, CRP impairs fibrinolysis via the production of substances which block the breakdown of plasminogen into plasmin, a fibrinolytic [11]. All of them are important factors that increase the susceptibility of the vascular walls to atherogenic processes in diabetic patients [12].
The next mechanism that contributes to atherogenesis and indirectly to the development of PAD is endothelial dysfunction due to hyperglycaemia, insulin resistance, and free fatty acid (FFA) production [13]. Another one is plaque instability, caused by the destructive effects of diabetes on the vascular smooth muscle cells (VSMCs) [14]. Those two are joined by platelet dysfunction, which can speed up atherosclerosis and have detrimental effects on plaque (destabilisation), promoting atherothrombosis [5, 15].
Diabetic patients usually have upregulated expression of platelet receptors, like glycoprotein Ib and IIb/IIIa receptors (essential to fibrin-platelet interaction) – they regulate platelet aggregation and adhesion and thus directly affect the induction of thrombosis [11]. Other platelet-related mechanisms that are disrupted in diabetic patients are intra-platelet calcium regulation and thromboxane production, further aggravating atherosclerosis [11, 16, 17, 18].
Diabetes, more specifically hyperglycaemia, encourages hypercoagulability through upregulation of tissue factor by endothelial cells and VSMCs and increases coagulation factor VIIA production while decreasing production of anticoagulants such as antithrombin and protein C [19, 20].
On top of that, diabetes also diminishes fibrinolytic function and at the same time promotes production of PAI-1 protein and together with other aforementioned abnormalities increases the risk of atherosclerotic plaque rupture, leading to possible thrombus formation [4, 20, 21, 22].
Physical properties of blood like viscosity are also anomalous (elevated) in diabetic patients, together with increased fibrinogen production – this usually manifests as abnormal Ankle-Brachial Index (ABI), essential information for accurate PAD diagnosis [4, 23].
Even patients who have had an angioplasty are at an increased risk of restenosis due to the harmful effects of hyperglycaemia on the production of monocyte chemoattractant-protein-1, TNF-α and CRP and its contribution to the induction of endothelial dysfunction and oxidative stress [24].
Last but not least, diabetes also impairs arteriogenesis, which is an important mechanism for restoring blood flow in response to an obstruction. The trigger is endothelial shear stress, detected by the vessel wall through integrins, adhesion molecules, tyrosine kinases and ion channels [25, 26, 27].
Diabetes inhibits the arteriogenesis mechanism by constricting the remodelling process itself: whether through weakening the sensing of shear stress, while enhancing the response to vasodilatory stimuli or by impairing the downstream signalling of monocytes, growth factor signalling and endothelial NO synthetase [28, 29, 30].
The detrimental effects of diabetes unfortunately do not end with merely increasing the incidence of PAD, but have profound impact on the course of both diseases. Poor glyacemic control is connected with higher risk of adverse outcomes in general (and, of course, incidence of PAD itself) and worse outcomes following vascular surgery (or endovascular intervention) [31].
Still, harmful effects can be mitigated (to a certain extent) by secondary risk (i.e. unhealthy lifestyle) reduction: smoking cessation, weight reduction, greater physical activity and healthy eating – diminishing severity of PAD and improving recovery post revascularisation [32].
The detrimental effects of diabetes on the cardiovascular system increase both incidence and severity of PAD, leading to greater morbidity and mortality and the necessity to screen diabetic patients for the disease on the basis of Ankle-Brachial Index (ABI) score before formulating any comprehensive treatment programme.