The impact of other factors on the treatment of Peripheral Arterial Disease (PAD)
Peripheral artery disease (PAD) is easy to prevent, but difficult to treat once it is already in the more advanced stage. Prevention is, of course, better than treatment, although awareness about this insidious disease, which is often asymptomatic, is still largely, at least on a global level, quite low, particularly when it comes to risk factors.
Just as for many other cardiovascular diseases (CVDs), some, particularly the major ones, risk factors are modifiable in nature, i.e. are within the patient’s influence to eliminate or at least mitigate them. However, as any physician or (psycho)therapist would testify, well-entrenched habits (diet, sedentary lifestyle, etc.) are hard to change or abruptly stop, especially if there is an underlying addiction mechanism.
The best example is tobacco smoking, the biggest modifiable risk factor for PAD and other CVDs. It is estimated that just in the year 2000, 1 out of every 10 deaths due to CVDs was related to smoking [1]. It is also a known fact that smoking cessation and continuous abstinence has many positive health benefits and can sometimes eliminate or at least greatly mitigate the risk of development of a myriad of diseases besides CVDs [2, 3, 4, 5, 6].
What should a primary care doctor consider when treating patients with Peripheral Arterial Disease (PAD)?
There are several stages of PAD, each of them progressively worse for the affected individual in both morbidity and mortality. In the beginning the patient might be entirely unaware of his condition since more than 40% of patients with PAD are entirely asymptomatic [7]. As the disease progresses, some might experience intermittent claudication (the most typical symptom of PAD), but even that is not a given as some might have rather severe atherosclerosis of the lower-extremity arteries without feeling any pain or discomfort, during physical exertion or otherwise. Alternatively, it can be misdiagnosed as sciatica, delaying proper treatment if there were no additional diagnostic steps undertaken such as taking an ABI measurement – the most cost effective and convenient way of diagnosing PAD. Learn more about the MESI mTABLET ABI
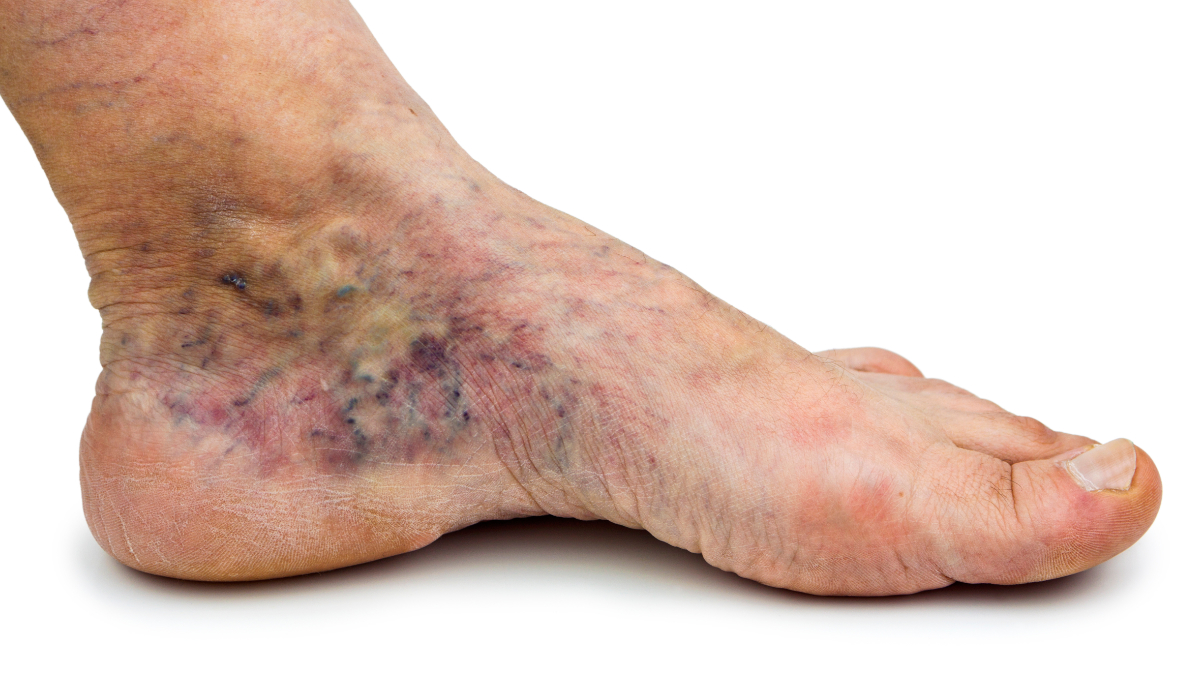
Proper diagnosis is naturally only the beginning of treatment, which should be conservative at the start, under the condition that PAD is not in the later stages and the patient already has arterial insufficiency ulcers (ischaemic ulcers) that are difficult and expensive to treat. They may even have critical limb ischaemia (CLI), which has a grave prognosis, including the possibility of an amputation. This is exactly what clinicians should be telling patients with PAD when discussing possible complications and the need to manage risk factors, most notably smoking. And there are plenty of well-researched statistics to back their claims.
The presence of PAD, diagnosed on the basis of an ABI measurement, is an important indicator of overall cardiovascular health and can improve the accuracy of cardiovascular risk prediction beyond the FRS (Framingham risk score) [8].
The connection between PAD and (cardiovascular) mortality is well established as individuals with the disease are subject to threefold greater risk of death (from all causes) than those without PAD [9]. The rationale behind this is the possible presence of atherosclerosis in other arterial beds besides those in the lower extremities, which explains comorbidity with other CVDs such as coronary artery disease (CAD).
It is estimated that 22 to 42% of patients with CAD, which is the biggest killer amongst CVDs and on its own, likewise have PAD and they fare worse (healthwise) than individuals with either [10, 11, 12, 13, 14]. Last but not least, the final stage of PAD – CLI – is associated with major amputation rates ranging from 10 to 40% in the 6-month period from diagnosis [15, 16]. Diagnosis of CLI as such is connected with up to 50% mortality rate in the 5-year period [17].
Smoking cessation
Smoking is recognised as the single biggest risk factor for the development of PAD for both genders, although it affects females far worse than males. The (overall) prevalence of symptomatic PAD is 2.3 times greater in current smokers in comparison with non-smokers and is, surprisingly 2.6 times greater in former smokers [18]. This harmful effect is so pronounced that it is estimated that the association between smoking and incidence of PAD is 2 to 3 times stronger in comparison with CAD incidence and smoking [19]. And speaking of particular harm for females: studies have shown that female smokers are 20 times more at risk than those who have never smoked [20].
Patients with PAD who are currently smoking should therefore be strongly encouraged to quit (not only because of PAD), but great care should be taken to do so in a gradual and controlled manner and actively guide the patient through the process. Guided (assisted) smoking cessation that entails behavioural support and counselling and medications is more effective than the individual’s own attempts without proper support [21]. Individuals who have stopped smoking have greatly reduced mortality and morbidity.
One study has shown that the 10-year survival rate for PAD patients was 82% in former smokers and just 46% in current smokers - i.e. current smokers were nearly two times more likely to die in that time period [22]. Former smokers have less severe forms of intermittent claudication, which manifests later than in current smokers and have better outcomes after vascular surgery [23, 24, 25, 26].
Hyperlipidaemia management
Abnormally high levels of lipids in blood are associated with a twofold increase in the risk of intermittent claudication [27]. Moreover, since PAD is indicative of overall cardiovascular health, hyperlipidaemia can exacerbate other co-existing (and possibly undiagnosed) CVDs like CAD and greatly contribute to coronary mortality [28, 29]. Possible treatment approaches include encouraging greater physical activity and exercising, and medications, such as statins – the former is more desirable as exercise has other benefits for PAD and a host of other conditions [30].
Hypertension management
Hypertension is also one of the risk factors for PAD (about 35 to 55% of patients are hypertensive) that responds well to physical exercise: even relatively moderate physical activity has beneficial effects and should be recommended to patients [31, 32]. However, when it comes managing hypertension in PAD patients through pharmacological means, the evidence of benefits of various anti-hypertensive medications is rather poor – this still does not detract from the need to manage hypertension since many patients have, in addition to PAD, other CVDs that benefit from this [33].
Managing risk factors such as tobacco smoking, hyperlipidaemia and hypertension in patients with PAD is of great importance, not just from the perspective of treating the disease itself, but also to prevent, mitigate and manage other cardiovascular issues.